Menopause is not only a personal issue —
it is a workforce, economic and public health issue.
At any given time, a significant proportion of women in midlife are navigating perimenopause or menopause — often while leading teams, managing households, and contributing at the highest levels of their organisations.

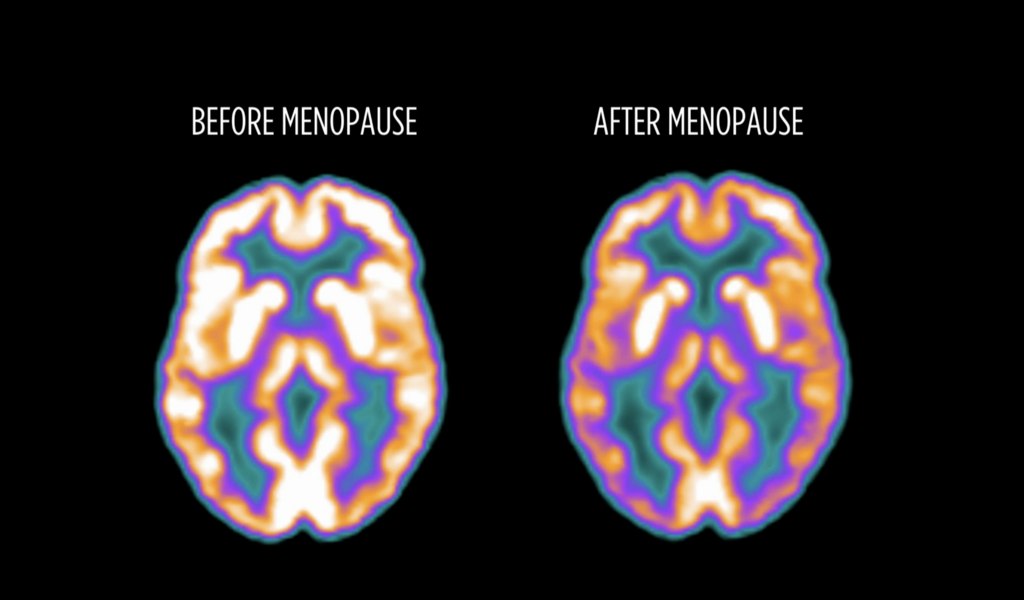
Menopause is not just a reproductive transition —
it is a neurological one.
Estrogen is far more than a reproductive hormone. It plays a central role in how the brain regulates memory, focus, mood, sleep, and temperature. Estrogen receptors are highly concentrated in key brain regions, including:
The hippocampus – responsible for memory formation and learning
The prefrontal cortex – governing focus, executive function, planning and decision-making
The amygdala – central to emotional processing and stress response
The hypothalamus – regulating temperature, sleep cycles and hormonal signalling
During perimenopause, estrogen levels fluctuate unpredictably. In menopause, levels decline more steadily. These hormonal shifts affect how these brain regions communicate and function — leading to the symptoms many women recognise:
This is not cognitive decline. It is neuroendocrine adaptation.
Research shows that the menopausal brain undergoes temporary shifts in glucose metabolism and neural connectivity. The brain is recalibrating. And importantly, it is highly adaptable. Many women report that after this transition phase, they experience improved emotional regulation, stronger boundaries, sharper prioritisation and renewed clarity.
Understanding menopause through a neurological lens changes the narrative.
This is not a loss of ability — it is a phase of brain reorganisation.
At INSIDEHER, we believe that when women understand what is happening in their brains, symptoms become less frightening, more manageable, and easier to address with the right support, lifestyle interventions, and (when appropriate) medical care.
Menopause is a biological transition — and the brain is at its centre.